Tuberous Sclerosis Complex (TSC)
Overview

Other Names & Coding
Q85.1, Tuberous sclerosis
ICD-10 for Tuberous Sclerosis (icd10data.com) provides further coding details.
Prevalence
Genetics
Mutations in TSC2 are more common than in TSC1 and are generally associated with more severe clinical presentations, although exceptions exist. [Peron: 2018] [Orlova: 2010] In families with TSC, mild and severe cases may appear within the same generation. Parents of a child with TSC could harbor a mutation of 1 of the 2 genes but not fulfill clinical diagnostic criteria. This reflects the variability of clinical expressivity of TSC and the possible low-level mosaicism in the unaffected parent who harbors either a TSC1 or TSC2 mutation. Studies have demonstrated that a portion of affected individuals carry mosaic mutations in either TSC1 or TSC2, which means that cells with the mutation and cells without the mutation co-exist in some patients.
Prognosis
Practice Guidelines
The following offer consensus recommendations from Tuberous Sclerosis Complex International (TSCi) for diagnostic criteria and management of TSC, updating recommendations published in 2013, and recommendations for closing the gap between the guidelines and available care.
Northrup H, Aronow ME, Bebin EM, Bissler J, Darling TN, de Vries PJ, Frost MD, Fuchs Z, Gosnell ES, Gupta N, Jansen AC, Jóźwiak
S, Kingswood JC, Knilans TK, McCormack FX, Pounders A, Roberds SL, Rodriguez-Buritica DF, Roth J, Sampson JR, Sparagana S,
Thiele EA, Weiner HL, Wheless JW, Towbin AJ, Krueger DA.
Updated International Tuberous Sclerosis Complex Diagnostic Criteria and Surveillance and Management Recommendations.
Pediatr Neurol.
2021;123:50-66.
PubMed abstract
Stuart C, Fladrowski C, Flinn J, Öberg B, Peron A, Rozenberg M, Smith CA.
Beyond the Guidelines: How We Can Improve Healthcare for People With Tuberous Sclerosis Complex Around the World.
Pediatr Neurol.
2021;123:77-84.
PubMed abstract
Roles of the Medical Home
Clinical Assessment
Pearls & Alerts for Assessment
COVID-19 update (as of January 2021)Little is known about people with genetic conditions and COVID-19, but useful resources and documents from key leaders in TSC clinical care can be found at Covid-19 & TSC Resources (Tuberous Sclerosis Alliance). A recent study from Europe (and an unpublished update) suggested that patients with TSC are not at increased risk of developing COVID-19, as the prevalence of SARS-CoV-2 infection and the outcomes in those who developed the disease overlap with those in the general population. However, people with multiple comorbidities remain at risk of worse outcomes. [Peron: 2020]
Consider TSC if cardiac tumor is identifiedPerinatal identification of cardiac tumor, especially in the intraventricular wall, should lead to consideration of TSC.
Infants with cardiac rhabdomyomasInfants with TSC may be very ill with respiratory distress, arrhythmias, and cardiomegaly due to cardiac rhabdomyomas.
SEGAs can cause neurologic problemsAbout 5-15% of children and adolescents have subependymal giant cell astrocytomas (SEGAs). Although they are benign tumors, they can cause serious neurologic problems, including hydrocephalus. Pay attention to unexplained changes in neurological status.
Hypomelanotic macules may not be visibleHypomelanotic macules may only be visible by Woods lamp skin examination, which can be done at subspecialty clinics during an evaluation of TSC if it is not available in the primary care setting.
Risk of TSC and autosomal dominant polycystic kidney diseaseA contiguous gene deletion encompassing both TSC2 and PKD1 causes both TSC and autosomal dominant polycystic kidney disease. These individuals have a higher risk than those with TSC alone of developing end-stage renal disease.
Genetic vs. clinical diagnosisOf the individuals who fulfill clinical diagnostic criteria, up to 10% do not have a documented molecular etiology. A negative genetic test does not exclude the diagnosis.
Screening
Of Family Members
For Complications
Presentations
Diagnostic Criteria
Genetic diagnostic criteria: The identification of either a TSC1 or TSC2 pathogenic mutation is sufficient to make a definite diagnosis. A pathogenic mutation is defined as a mutation that clearly inactivates either tuberin or hamartin or disrupts their respective functional activity.
Clinical diagnostic criteria: [Northrup: 2021]
Definite TSC - 2 major features, or 1 major feature plus 2 or more minor features
Possible TSC - 1 major feature, or 2 or more minor features
Major features:
- Hypomelanotic macules (≥3, at least 5-mm in diameter)
- Angiofibromas (≥3) or fibrous cephalic plaque
- Ungual fibromas (≥2)
- Shagreen patch
- Multiple retinal hamartomas
- Tubers and cerebral white matter radial migration lines
- Subependymal nodules
- Subependymal giant cell astrocytoma (SEGA)
- Cardiac rhabdomyoma
- Lymphangioleiomyomatosis (LAM)
- Renal angiomyolipoma (AMLs) (≥2)

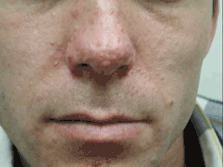
Minor features
- Dental enamel pits (≥3)
- Intraoral fibromas (≥2)
- Nonrenal hamartoma
- Retinal achromic patch
- "Confetti" skin lesions
- Multiple renal cysts
- Sclerotic bone lesions
Differential Diagnosis
Comorbid & Secondary Conditions
Brain manifestations include cortical tubers, subependymal nodules, SEGAs, and seizures. Some evidence suggests that the number of tubers correlates with the degree of intellectual disability and the number of seizures. [Goodman: 1997] Subependymal nodules (<1 cm) are present in 80% of patients but don’t cause clinical problems. SEGAs are subependymal nodules that are >1 cm and located near the Foramen of Monro. They occur in 5-15% of the patients and rarely develop after 25 years of age. They may enlarge and cause hydrocephalus by obstructing the ventricular CSF outflow system and result in morbidity and death.
Seizures, especially infantile spasms and/or focal seizures, occur in more than 80% of individuals with TSC and, rarely, may be life-threatening. [Asato: 2004] Complications, such as status epilepticus and pneumonia leading to respiratory failure, are leading causes of early death in individuals with TSC. In nearly half of the patients, seizures can be treatment resistant. A combination of more than one antiepileptic drug might be necessary for adequate control. Vigabatrin is the recommended first-line treatment for infantile spasms. Its use has been associated with better outcomes related to seizures and cognitive abilities. [Camposano: 2008]
TAND describes all the TSC-associated neuropsychiatric disorders that occur in up to 90% of patients, regardless of age. These challenges encompass behavioral (aggression, tantrums, sleep problems), psychiatric (autism spectrum disorder, ADHD), intellectual (intellectual disability), academic (learning difficulties), neuropsychological (memory recall, dual-tasking), and psychosocial (self-esteem, relationship) difficulties. [de: 2015] Developmental delay/intellectual disability (ID) is present in 50% of individuals with TSC, and 30% have profound ID. Specific learning difficulties are common in individuals whose IQ is in the normal range. Autism spectrum disorder has been reported in 17-61% of people with TSC. [Curatolo: 2004] In a survey, cognitive and behavioral issues were the manifestations of TSC that caused parents the most concern. [Prather: 2004]
Kidney problems include AMLs and cysts. The majority of pre-teens with TSC have at least 1 renal lesion that tends to increase in size and number with time. Larger AMLs (>4cm in diameter) may abruptly bleed and become life-threatening, or they may replace normal renal tissue and lead to end-stage renal disease.
Heart problems include rhabdomyomas, which are generally present in infancy and regress spontaneously. They can cause arrhythmias in a minority of newborns but require treatment only if they cause ventricular outlet obstruction.
LAM may occur; usually, it is seen only in adult females.
Ophthalmological complications, such as retinal hamartomas and retinal hypopigmented patches, are usually clinically benign and don’t cause visual impairment. [Tuberous: 2006]
History & Examination
Current & Past Medical History
Family History
Pregnancy/Perinatal History
Developmental & Educational Progress
Social & Family Functioning
Physical Exam
Skin
HEENT/Oral
Eye manifestations may include hypopigmented areas of the retina and retinal hamartomas. Teeth may have pitting. Intraoral fibromas may be present.
Chest
Screen for possible signs of LAM (exertional dyspnea, shortness of breath) in adolescent and adult women.
Testing
Sensory Testing
- Although eye manifestations do not generally affect visual acuity, the initial evaluation should include a visual evaluation with dilated fundoscopy.
- Children require ophthalmological screening before starting vigabatrin due to the chance of developing constriction of the visual fields. Then screen at periodic intervals and after cessation. This should be arranged by the pediatric neurologist who initiates the medication.
Laboratory Testing
- Depending on the antiepileptic medication, children with seizures may need drug levels and/or other blood tests. Responsibility for monitoring may be worked out with the pediatric neurologist who initiated the medication.
- Assess renal function annually with serum creatinine and urinalysis.
Imaging
- Brain MRI at baseline to identify cortical tubers, subependymal nodules, and SEGAs. Repeat every 1-3 years in patients younger than age 25 years to monitor for new occurrence of SEGAs. Patients with a growing or even asymptomatic SEGA should have brain MRI as indicated for signs of increased intracranial pressure (frequency of scans in recommended range should be clinically determined).
- Renal ultrasound (or abdominal MRI, when possible) every 1-3 years through lifetime to detect renal cysts and AMLs, as well as other nonrenal hamartomas. The frequency of imaging is based on presence and size of lesions; MRI should be performed if larger lesions are found.
- High-resolution, low-radiation CT (computed tomography) scan of the chest every 5-10 years in adult women to identify LAM
- Echocardiography every 1-3 years, or as indicated, in pediatric patients with cardiac rhabdomyoma until regression of the tumor
Genetic Testing
Other Testing
- An EKG and echocardiogram should be performed at diagnosis. An EKG should be repeated every 3-5 years in asymptomatic children and adults.
- A baseline EEG should be performed in all children upon diagnosis, especially in infants. EEG monitoring allows early detection of subclinical seizure activity and allows consideration of preventive treatment. [Curatolo: 2012] The frequency of follow-up EEGs in individuals with known seizures should be determined by the pediatric neurologist based on clinical needs.
- Periodic neuropsychological and achievement testing should be performed through the school to assess progress and identify opportunities for focused interventions.
- Adult women should receive pulmonary function testing.
Specialty Collaborations & Other Services
Medical Genetics (see NW providers [1])
Pediatric Neurology (see NW providers [0])
Developmental - Behavioral Pediatrics (see NW providers [1])
Pediatric Nephrology (see NW providers [0])
Pediatric Ophthalmology (see NW providers [1])
Pediatric Pulmonology (see NW providers [0])
Sleep Study/Polysomnography (see NW providers [0])
Pediatric Dermatology (see NW providers [1])
Treatment & Management
Pearls & Alerts for Treatment & Management
Evaluate children on vigabatrin for retinal toxicityChildren on vigabatrin need frequent ophthalmological evaluations for retinal toxicity. Evaluations will generally be arranged by the pediatric neurologist.
Evaluate onset of new headaches promptlyPeriodically screen for SEGAs using MRI. Image children with new headaches, particularly if the headaches are accompanied by vomiting.
Consider mTOR inhibitorsEverolimus and sirolimus are effective in reducing the size of growing SEGAs and renal AMLs, stabilizing lung function, and reducing the size of lymphangioleiomyomas. Everolimus has also been approved for the adjunctive treatment of refractory focal-onset seizures in patients older than 2 years of age. Off-label use has shown encouraging results in treating symptomatic cardiac rhabdomyomas and facial angiofibromas (as a topical formulation). [Northrup: 2021]
How should common problems be managed differently in children with Tuberous Sclerosis Complex (TSC)?
Introduction
Development (Cognitive, Motor, Language, Social-Emotional)
Prescription Medications
Everolimus has been demonstrated to reduce seizures in patients with refractory focal-onset seizures. [French: 2016] The use of Cannabidiol in patients with TSC is currently being evaluated. [Thiele: 2020]
mTOR inhibitors (everolimus and sirolimus) are effective in reducing the size of growing SEGAs and renal AMLs >3 cm. [Franz: 2013] [Bissler: 2013] Everolimus is FDA-approved in adults and children ≥ 3 years of age for SEGAs, in adults for renal AMLs, and in adults and children ≥2 years of age as adjunctive treatment for refractory focal-onset seizures. Sirolimus is FDA-approved to treat LAM. Due to possible side effects (increased risk of infections, stomatitis, elevation of blood glucose, triglycerides, and cholesterol), use only the minimum effective dose, monitor for side effects, and monitor drug serum levels. Prescribing physicians should be aware that treatment might be lifelong since tumor regrowth has been noticed after treatment discontinuation. [Curatolo: 2016]
mTOR inhibitors also show promise in treating other manifestations of TSC, such as non-renal hamartomas, cardiac rhabdomyomas, and facial angiofibromas (topical formulations); however, rapalogs are not yet approved for these indications.
Adolescent and adult women of childbearing age should be counseled regarding estrogen use because estrogen can worsen LAM.
Other
Systems
Development (general)
Children with TSC should have initial developmental and behavioral assessments and then be placed in early childhood intervention programs for therapies (PT, OT, speech) to address specific delays. Reassessments should be performed at regular intervals; IQ and achievement testing should be performed during the preschool and school-age years. Treat seizures as rapidly and completely as possible (see Neurology, below). Early control of TSC-associated seizures, particularly infantile spasms, is associated with improved neurodevelopmental outcomes. [Bombardieri: 2010]
The Portal modules for Intellectual Disability & Global Developmental Delay, Attention-Deficit/Hyperactivity Disorder (ADHD), Autism Spectrum Disorder, Depression, and Infantile Spasms provide diagnosis and management information for these conditions.
Specialty Collaborations & Other Services
Developmental - Behavioral Pediatrics (see NW providers [1])
Early Intervention for Children with Disabilities/Delays (see NW providers [3])
Preschools (see NW providers [0])
Neuropsychiatry/Neuropsychology (see NW providers [0])
Physical Therapy (see NW providers [0])
Occupational Therapy (see NW providers [1])
Speech - Language Pathologists (see NW providers [4])
Neurology
SEGAs are subependymal nodules that arise near the Monro foramina, which connect the lateral ventricles and the third ventricle. When SEGAs become large enough, they can block the flow of cerebrospinal fluid, leading to hydrocephalus and, if untreated, death. Treatment usually involves close surveillance and removal of enlarging tumors or use of mTOR inhibitors to shrink the tumors before signs of increased intracranial pressure appear. [Berhouma: 2010]
Everolimus and sirolimus, which inhibit the activated mTOR pathway involved in cell proliferation, have been approved for treating SEGAs in both children and adults. [Franz: 2013] Periodic screening for SEGAs is accomplished using MRI, but children with new headaches, particularly accompanied by vomiting, should be imaged acutely. In the absence of new medical or behavior concerns, brain MRI with and without gadolinium is recommended every 1 to 3 years until age 25.
Seizures affect between 65-95% of individuals with TSC; refractory seizures, 20-50%. Seizure frequency may be related to the number of cortical tubers; however, it is probably not the cortical tubers but the surrounding tissue that is epileptogenic. [Major: 2009] Seizures often manifest as infantile spasms, which can be difficult to treat and may be life-threatening. Vigabatrin is currently the drug of choice for infantile spasms associated with TSC, even though there may be retinal toxicity. Because vigabatrin can cause permanent peripheral visual field loss (thought to be due to drug-induced injury to photoreceptors and retinal ganglion cells and their axons), children require ophthalmological screening before starting vigabatrin and then at periodic intervals and after cessation. Screening should be arranged by the pediatric neurologist who initiates the medication. [Kossoff: 2010] Adrenocorticotropic hormone (ACTH) and topiramate may also be used to control infantile spasms, depending on pediatric neurology preference and expertise. In children with localizable foci of epileptogenic activity, surgery may be helpful. Another common type of seizure, focal seizures, can present at any age. Infantile spasms, earlier age at seizure onset, and drug resistance are usually associated with a worse cognitive outcome, making prompt and appropriate treatment crucial.
Specialty Collaborations & Other Services
Pediatric Neurology (see NW providers [0])
Pediatric Hematology/Oncology (see NW providers [2])
Pediatric Neurosurgery (see NW providers [1])
Renal
Typically, surveillance consists of renal ultrasounds or abdominal MRI (preferred), every 1-3 years, in individuals without known lesions. Increase frequency of ultrasounds or MRI for those with numerous or larger lesions. MRI of the abdomen provides better resolution for AMLs and should be performed in conjunction with brain MRI in older prepubertal children to prepare for potential growth in adolescence. Depending on their location, large AMLs (>3.5 cm) may be removed prophylactically by renal embolization or partial nephrectomy to prevent hemorrhage into the tumor and pain. Blood pressure monitoring at every clinical visit is recommended, and enhanced renal function monitoring is indicated for those with renal lesions. [Seyam: 2008] mTOR inhibitors are approved and considered the first-line treatment for renal AMLs >3 cm in adults. [Bissler: 2016]
Specialty Collaborations & Other Services
Pediatric Nephrology (see NW providers [0])
Mental Health/Behavior
Specialty Collaborations & Other Services
Developmental - Behavioral Pediatrics (see NW providers [1])
Mental Health Evaluation/Assessment (see NW providers [0])
Neuropsychiatry/Neuropsychology (see NW providers [0])
Behavioral Therapies (see NW providers [1])
Pediatric Neurology (see NW providers [0])
Psychiatry/Medication Management (see NW providers [0])
Cardiology
Specialty Collaborations & Other Services
Pediatric Cardiology (see NW providers [0])
Respiratory
Specialty Collaborations & Other Services
Pediatric Pulmonology (see NW providers [0])
Maturation/Sexual/Reproductive
Specialty Collaborations & Other Services
Gynecology: Pediatric/Adolescent; Special Needs (see NW providers [0])
Skin & Appearance
Specialty Collaborations & Other Services
Pediatric Dermatology (see NW providers [1])
Pediatric Ophthalmology (see NW providers [1])
Learning/Education/Schools
Ask the Specialist
If I suspect TSC, what testing should I send?
The diagnosis of TSC is based on established diagnostic criteria (listed above). [Northrup: 2013] Genetic testing can be useful in uncertain cases and for screening family members once the pathogenic mutation has been identified. Consider starting with mutation analysis of TSC1 and TSC2 using next generation sequencing and, if negative, request deletion/duplication analysis of both genes. About half of the patients with a mutation that was not identified in the past carry a mosaic mutation in TSC1 or TSC2. Therefore, re-testing with newer molecular techniques may be warranted if patients were tested before 2015. A mutation cannot be identified in up to 10% of patients, but this does not exclude the diagnosis.
In general, what is the minimum medical work-up to do after diagnosis of TSC?
Since TSC is a multisystemic condition, the initial studies should be aimed at determining the extent of the disease and organ involvement. Testing should include brain MRI, EEG, pediatric neurology evaluation, pediatric ophthalmology evaluation with fundoscopy, echocardiography/ECG, abdominal ultrasound/MRI, genetic evaluation (with assessment of skin findings, if dermatology is not available), and screens for TSC-associated neuropsychiatric disorders.
Will all patients with TSC develop intellectual disability?
No, while about half of the patients diagnosed with TSC have intellectual disability, which can vary from mild to profound, the other half have normal cognitive functioning. Some of these individuals, though, can experience specific learning or behavioral difficulties. Remember, there is a high clinical variability, even within the same family.
What are the most effective therapies for TSC?
Treatment in TSC is multidisciplinary and involves all specialists. Vigabatrin is the first-line treatment for infantile spasms, but possible visual side effects should be monitored. mTOR inhibitors (everolimus and sirolimus) are useful in treating SEGAs, renal AMLs, and LAM. They also are showing promising results in leading to regression of other TSC-related tumors. Side effects are generally well-tolerated, but the treatment might be lifelong.
Resources for Clinicians
On the Web
Tuberous Sclerosis Complex (GeneReviews)
Detailed information addressing clinical characteristics, diagnosis/testing, management, genetic counseling, and molecular
pathogenesis; from the University of Washington and the National Library of Medicine.
Tuberous Sclerosis 1 (OMIM)
Information about clinical features, diagnosis, management, and molecular and population genetics; Online Mendelian Inheritance
in Man, authored and edited at the McKusick-Nathans Institute of Genetic Medicine, Johns Hopkins University School of Medicine
Tuberous Sclerosis 2 (OMIM)
Information about clinical features, diagnosis, management, and molecular and population genetics; Online Mendelian Inheritance
in Man, authored and edited at the McKusick-Nathans Institute of Genetic Medicine, Johns Hopkins University School of Medicine
Skin Findings in TSC (TSAlliance.org)
Information and photos for classic cutaneous manifestations of TSC that include hypomelanotic macules, facial angiofibromas,
and shagreen patch.
The LAM Foundation
Nonprofit organization that offers information, resources, and grants for research related to lymphangioleiomyomatosis (LAM).
The Healthcare Providers tab on the top of the page provides clinical diagnosis and management information. Other tabs provide
information and resources for families affected by LAM and TSC.
Helpful Articles
PubMed search for tuberous sclerosis complex in children, last 4 years.
Curatolo P, Jóźwiak S, Nabbout R.
Management of epilepsy associated with tuberous sclerosis complex (TSC): clinical recommendations.
Eur J Paediatr Neurol.
2012;16(6):582-6.
PubMed abstract
Jansen AC, Vanclooster S, de Vries PJ, Fladrowski C, Beaure d'Augères G, Carter T, Belousova E, Benedik MP, Cottin V, Curatolo
P, Dahlin M, D'Amato L, Ferreira JC, Feucht M, Hertzberg C, Jozwiak S, Lawson JA, Macaya A, Marques R, Nabbout R, O'Callaghan
F, Qin J, Sander V, Sauter M, Shah S, Takahashi Y, Touraine R, Youroukos S, Zonnenberg B, Kingswood JC.
Burden of Illness and Quality of Life in Tuberous Sclerosis Complex: Findings From the TOSCA Study.
Front Neurol.
2020;11:904.
PubMed abstract / Full Text
de Vries PJ, Belousova E, Benedik MP, Carter T, Cottin V, Curatolo P, Dahlin M, D'Amato L, Beaure d'Augères G, Ferreira JC,
Feucht M, Fladrowski C, Hertzberg C, Jozwiak S, Lawson JA, Macaya A, Marques R, Nabbout R, O'Callaghan F, Qin J, Sander V,
Sauter M, Shah S, Takahashi Y, Touraine R, Youroukos S, Zonnenberg B, Kingswood JC, Jansen AC.
Tuberous Sclerosis Complex-Associated Neuropsychiatric Disorders (TAND): New Findings on Age, Sex, and Genotype in Relation
to Intellectual Phenotype.
Front Neurol.
2020;11:603.
PubMed abstract / Full Text
Henske EP, Jóźwiak S, Kingswood JC, Sampson JR, Thiele EA.
Tuberous sclerosis complex.
Nat Rev Dis Primers.
2016;2:16035.
PubMed abstract
Manohara D.
Primary care management of tuberous sclerosis complex in children.
J Am Acad Nurse Pract.
2012;24(7):391-9.
PubMed abstract / Full Text
Jülich K, Sahin M.
Mechanism-Based Treatment in Tuberous Sclerosis Complex.
Pediatr Neurol.
2013.
PubMed abstract
Wataya-Kaneda M, Tanaka M, Hamasaki T, Katayama I.
Trends in the prevalence of tuberous sclerosis complex manifestations: an epidemiological study of 166 Japanese patients.
PLoS One.
2013;8(5):e63910.
PubMed abstract / Full Text
Clinical Tools
Clinical Checklists & Visit Tools
TSC-Associated Neuropsychiatric Disorders (TAND) Checklist
A 12-question checklist designed to help guide decisions about further evaluation or treatment; offered for free download
by Tuberous Sclerosis Complex International.
Letters of Medical Necessity
Letter of Medical Necessity for TSC - Sample ( 18 KB)
18 KB)
Template that may be downloaded and edited to secure pre-authorization from insurance companies for diagnosis and management
of TSC; Medical Home Portal.
Patient Education & Instructions
An Introduction to TSC (Tuberous Sclerosis Alliance) ( 2.1 MB)
2.1 MB)
A 32-page online booklet that provides information about diagnosis, features, genetics, and support systems for families affected
by TSC.
TSC Patient Education Resources (Herscot Center, MGH)
Offers a variety of relevant information and family stories; from the Herscot Center for Tuberous Sclerosis Complex at Massachusetts
General Hospital.
Resources for Patients & Families
Information on the Web
Tuberous Sclerosis Information Page (NINDS)
Overview of TSC with emphasis on research and inclusion of links to studies and clinical trials; National Institute of Neurological
Disorders and Stroke.
Tuberous Sclerosis (Medline Plus)
Overview with links to reliable sources of more detailed information; from the National Library of Medicine.
Genetic Conditions: Tuberous Sclerosis (MedlinePlus)
Excellent, detailed review of the condition for patients and families; National Library of Medicine and National Institutes
of Health.
Tuberous Sclerosis (GARD)
Includes information about symptoms, inheritance, diagnosis, finding a specialist, related diseases, and support organizations;
Genetic and Rare Diseases Information Center of the National Center for Advancing Translational Sciences.
The LAM Foundation
Nonprofit organization that offers information, resources, and grants for research related to lymphangioleiomyomatosis (LAM).
The Healthcare Providers tab on the top of the page provides clinical diagnosis and management information. Other tabs provide
information and resources for families affected by LAM and TSC.
National & Local Support
Tuberous Sclerosis Alliance Support Community
An online support community for individuals and families affected by TSC; sponsored by Inspire.com - membership required.
TSC Community Alliances (TSAlliance.org)
Locations of volunteer groups who work with the TS Alliance to facilitate local connections for individuals and families affected
by TSC.
Tuberous Sclerosis (NORD)
Information for families that includes synonyms, signs & symptoms, causes, affected populations, related disorders, diagnosis,
therapies (both standard and investigational), and support organizations; National Organization of Rare Disorders.
Studies/Registries
Tuberous Sclerosis (clinicaltrials.gov)
Studies looking at better understanding, diagnosing, and treating this condition; from the National Library of Medicine.
Clinical Trials/Studies Related to TSC (TSAlliance.org)
A list compiled and maintained by the Tuberous Sclerosis Alliance with clinical trials and clinical studies that have obtained
Institutional Review Board approval.
Services for Patients & Families Nationwide (NW)
| Service Categories | # of providers* in: | NW | Partner states (4) (show) | | NM | NV | RI | UT | |
|---|---|---|---|---|---|---|---|---|---|
| Applied Behavior Analysis (ABA) | 2 | 17 | 11 | 27 | 62 | ||||
| Autism Programs | 1 | 7 | 2 | 4 | 56 | ||||
| Behavioral Therapies | 1 | 17 | 19 | 32 | 36 | ||||
| Developmental - Behavioral Pediatrics | 1 | 2 | 3 | 12 | 9 | ||||
| Early Intervention for Children with Disabilities/Delays | 3 | 34 | 30 | 13 | 51 | ||||
| Gynecology: Pediatric/Adolescent; Special Needs | 3 | 9 | |||||||
| Medical Genetics | 1 | 2 | 5 | 4 | 7 | ||||
| Mental Health Evaluation/Assessment | 8 | 9 | 24 | 131 | |||||
| Neuropsychiatry/Neuropsychology | 1 | 3 | 9 | 6 | |||||
| Occupational Therapy | 1 | 17 | 22 | 22 | 37 | ||||
| Pediatric Cardiology | 3 | 4 | 17 | 4 | |||||
| Pediatric Dermatology | 1 | 3 | 1 | 3 | 2 | ||||
| Pediatric Hematology/Oncology | 2 | 4 | 7 | 11 | 4 | ||||
| Pediatric Nephrology | 2 | 2 | 10 | 1 | |||||
| Pediatric Neurology | 5 | 5 | 18 | 8 | |||||
| Pediatric Neurosurgery | 1 | 2 | 4 | 3 | 2 | ||||
| Pediatric Ophthalmology | 1 | 6 | 6 | 8 | 4 | ||||
| Pediatric Pulmonology | 4 | 4 | 6 | 3 | |||||
| Physical Therapy | 12 | 9 | 7 | 40 | |||||
| Preschools | 6 | 33 | 10 | 71 | |||||
| Psychiatry/Medication Management | 3 | 37 | 80 | 53 | |||||
| Sleep Study/Polysomnography | 2 | 1 | 4 | ||||||
| Speech - Language Pathologists | 4 | 23 | 11 | 34 | 65 | ||||
For services not listed above, browse our Services categories or search our database.
* number of provider listings may vary by how states categorize services, whether providers are listed by organization or individual, how services are organized in the state, and other factors; Nationwide (NW) providers are generally limited to web-based services, provider locator services, and organizations that serve children from across the nation.
Authors & Reviewers
| Author: | Angela Peron, MD |
| Reviewer: | David Viskochil, MD, PhD |
| 2021: update: Angela Peron, MDA |
| 2016: update: Angela Peron, MDA; David Viskochil, MD, PhDR |
| 2014: update: David Viskochil, MD, PhDA |
| 2014: first version: Lynne M. Kerr, MD, PhDA |
Bibliography
Asato MR, Hardan AY.
Neuropsychiatric problems in tuberous sclerosis complex.
J Child Neurol.
2004;19(4):241-9.
PubMed abstract
Berhouma M.
Management of subependymal giant cell tumors in tuberous sclerosis complex: the neurosurgeon's perspective.
World J Pediatr.
2010;6(2):103-10.
PubMed abstract
Bissler JJ, Kingswood JC, Radzikowska E, Zonnenberg BA, Frost M, Belousova E, Sauter M, Nonomura N, Brakemeier S, de Vries
PJ, Berkowitz N, Miao S, Segal S, Peyrard S, Budde K.
Everolimus for renal angiomyolipoma in patients with tuberous sclerosis complex or sporadic lymphangioleiomyomatosis: extension
of a randomized controlled trial.
Nephrol Dial Transplant.
2016;31(1):111-9.
PubMed abstract
Bissler JJ, Kingswood JC, Radzikowska E, Zonnenberg BA, Frost M, Belousova E, Sauter M, Nonomura N, Brakemeier S, de Vries
PJ, Whittemore VH, Chen D, Sahmoud T, Shah G, Lincy J, Lebwohl D, Budde K.
Everolimus for angiomyolipoma associated with tuberous sclerosis complex or sporadic lymphangioleiomyomatosis (EXIST-2): a
multicentre, randomised, double-blind, placebo-controlled trial.
Lancet.
2013;381(9869):817-24.
PubMed abstract
Bombardieri R, Pinci M, Moavero R, Cerminara C, Curatolo P.
Early control of seizures improves long-term outcome in children with tuberous sclerosis complex.
Eur J Paediatr Neurol.
2010;14(2):146-9.
PubMed abstract
Burke A, Virmani R.
Pediatric heart tumors.
Cardiovasc Pathol.
2008;17(4):193-8.
PubMed abstract
Camposano SE, Major P, Halpern E, Thiele EA.
Vigabatrin in the treatment of childhood epilepsy: a retrospective chart review of efficacy and safety profile.
Epilepsia.
2008;49(7):1186-91.
PubMed abstract
Chu-Shore CJ, Major P, Camposano S, Muzykewicz D, Thiele EA.
The natural history of epilepsy in tuberous sclerosis complex.
Epilepsia.
2010;51(7):1236-41.
PubMed abstract / Full Text
Cleary A, McMahon CJ.
Literature review of international mammalian target of rapamycin inhibitor use in the non-surgical management of haemodynamically
significant cardiac rhabdomyomas.
Cardiol Young.
2020;30(7):923-933.
PubMed abstract
Colaneri M, Quarti A, Pozzi M.
Everolimus-induced near-resolution of giant cardiac rhabdomyomas and large renal angiomyolipoma in a newborn with tuberous
sclerosis complex.
Cardiol Young.
2016;26(5):1025-8.
PubMed abstract
Curatolo P, Bjørnvold M, Dill PE, Ferreira JC, Feucht M, Hertzberg C, Jansen A, Jóźwiak S, Kingswood JC, Kotulska K, Macaya
A, Moavero R, Nabbout R, Zonnenberg BA.
The Role of mTOR Inhibitors in the Treatment of Patients with Tuberous Sclerosis Complex: Evidence-based and Expert Opinions.
Drugs.
2016;76(5):551-65.
PubMed abstract
Curatolo P, Jóźwiak S, Nabbout R.
Management of epilepsy associated with tuberous sclerosis complex (TSC): clinical recommendations.
Eur J Paediatr Neurol.
2012;16(6):582-6.
PubMed abstract
Curatolo P, Porfirio MC, Manzi B, Seri S.
Autism in tuberous sclerosis.
Eur J Paediatr Neurol.
2004;8(6):327-32.
PubMed abstract
D'Agati E, Moavero R, Cerminara C, Curatolo P.
Attention-deficit hyperactivity disorder (ADHD) and tuberous sclerosis complex.
J Child Neurol.
2009;24(10):1282-7.
PubMed abstract
de Vries PJ, Belousova E, Benedik MP, Carter T, Cottin V, Curatolo P, Dahlin M, D'Amato L, Beaure d'Augères G, Ferreira JC,
Feucht M, Fladrowski C, Hertzberg C, Jozwiak S, Lawson JA, Macaya A, Marques R, Nabbout R, O'Callaghan F, Qin J, Sander V,
Sauter M, Shah S, Takahashi Y, Touraine R, Youroukos S, Zonnenberg B, Kingswood JC, Jansen AC.
Tuberous Sclerosis Complex-Associated Neuropsychiatric Disorders (TAND): New Findings on Age, Sex, and Genotype in Relation
to Intellectual Phenotype.
Front Neurol.
2020;11:603.
PubMed abstract / Full Text
de Vries PJ, Whittemore VH, Leclezio L, Byars AW, Dunn D, Ess KC, Hook D, King BH, Sahin M, Jansen A.
Tuberous sclerosis associated neuropsychiatric disorders (TAND) and the TAND Checklist.
Pediatr Neurol.
2015;52(1):25-35.
PubMed abstract / Full Text
Eden KE, de Vries PJ, Moss J, Richards C, Oliver C.
Self-injury and aggression in tuberous sclerosis complex: cross syndrome comparison and associated risk markers.
J Neurodev Disord.
2014;6(1):10.
PubMed abstract / Full Text
Franz DN, Belousova E, Sparagana S, Bebin EM, Frost M, Kuperman R, Witt O, Kohrman MH, Flamini JR, Wu JY, Curatolo P, de Vries
PJ, Whittemore VH, Thiele EA, Ford JP, Shah G, Cauwel H, Lebwohl D, Sahmoud T, Jozwiak S.
Efficacy and safety of everolimus for subependymal giant cell astrocytomas associated with tuberous sclerosis complex (EXIST-1):
a multicentre, randomised, placebo-controlled phase 3 trial.
Lancet.
2013;381(9861):125-32.
PubMed abstract
French JA, Lawson JA, Yapici Z, Ikeda H, Polster T, Nabbout R, Curatolo P, de Vries PJ, Dlugos DJ, Berkowitz N, Voi M, Peyrard
S, Pelov D, Franz DN.
Adjunctive everolimus therapy for treatment-resistant focal-onset seizures associated with tuberous sclerosis (EXIST-3): a
phase 3, randomised, double-blind, placebo-controlled study.
Lancet.
2016;388(10056):2153-2163.
PubMed abstract
Goodman M, Lamm SH, Engel A, Shepherd CW, Houser OW, Gomez MR.
Cortical tuber count: a biomarker indicating neurologic severity of tuberous sclerosis complex.
J Child Neurol.
1997;12(2):85-90.
PubMed abstract
Günther T, Schreiber C, Noebauer C, Eicken A, Lange R.
Treatment strategies for pediatric patients with primary cardiac and pericardial tumors: a 30-year review.
Pediatr Cardiol.
2008;29(6):1071-6.
PubMed abstract
Henske EP, Jóźwiak S, Kingswood JC, Sampson JR, Thiele EA.
Tuberous sclerosis complex.
Nat Rev Dis Primers.
2016;2:16035.
PubMed abstract
Hong CH, Tu HP, Lin JR, Lee CH.
An estimation of the incidence of tuberous sclerosis complex by a nationwide retrospective cohort study from 1997 to 2010.
Br J Dermatol.
2016.
PubMed abstract
Isaacs H.
Perinatal (fetal and neonatal) tuberous sclerosis: a review.
Am J Perinatol.
2009;26(10):755-60.
PubMed abstract
Jansen AC, Vanclooster S, de Vries PJ, Fladrowski C, Beaure d'Augères G, Carter T, Belousova E, Benedik MP, Cottin V, Curatolo
P, Dahlin M, D'Amato L, Ferreira JC, Feucht M, Hertzberg C, Jozwiak S, Lawson JA, Macaya A, Marques R, Nabbout R, O'Callaghan
F, Qin J, Sander V, Sauter M, Shah S, Takahashi Y, Touraine R, Youroukos S, Zonnenberg B, Kingswood JC.
Burden of Illness and Quality of Life in Tuberous Sclerosis Complex: Findings From the TOSCA Study.
Front Neurol.
2020;11:904.
PubMed abstract / Full Text
Jóźwiak S, Sadowski K, Kotulska K, Schwartz RA.
Topical Use of Mammalian Target of Rapamycin (mTOR) Inhibitors in Tuberous Sclerosis Complex-A Comprehensive Review of the
Literature.
Pediatr Neurol.
2016.
PubMed abstract
Jülich K, Sahin M.
Mechanism-Based Treatment in Tuberous Sclerosis Complex.
Pediatr Neurol.
2013.
PubMed abstract
Koenig MK, Bell CS, Hebert AA, Roberson J, Samuels JA, Slopis JM, Tate P, Northrup H.
Efficacy and Safety of Topical Rapamycin in Patients With Facial Angiofibromas Secondary to Tuberous Sclerosis Complex: The
TREATMENT Randomized Clinical Trial.
JAMA Dermatol.
2018;154(7):773-780.
PubMed abstract / Full Text
Kossoff EH.
Infantile spasms.
Neurologist.
2010;16(2):69-75.
PubMed abstract
Kotulska K, Kwiatkowski DJ, Curatolo P, Weschke B, Riney K, Jansen F, Feucht M, Krsek P, Nabbout R, Jansen AC, Wojdan K, Sijko
K, Głowacka-Walas J, Borkowska J, Sadowski K, Domańska-Pakieła D, Moavero R, Hertzberg C, Hulshof H, Scholl T, Benova B, Aronica
E, de Ridder J, Lagae L, Jóźwiak S.
Prevention of Epilepsy in Infants with Tuberous Sclerosis Complex in the EPISTOP Trial.
Ann Neurol.
2021;89(2):304-314.
PubMed abstract
Krueger DA, Northrup H.
Tuberous sclerosis complex surveillance and management: recommendations of the 2012 International Tuberous Sclerosis Complex
Consensus Conference.
Pediatr Neurol.
2013;49(4):255-65.
PubMed abstract / Full Text
Evidence-based, standardized approach for optimal clinical care provided for individuals with tuberous sclerosis complex.
Leclezio L, Jansen A, Whittemore VH, de Vries PJ.
Pilot validation of the tuberous sclerosis-associated neuropsychiatric disorders (TAND) checklist.
Pediatr Neurol.
2015;52(1):16-24.
PubMed abstract
Major P, Rakowski S, Simon MV, Cheng ML, Eskandar E, Baron J, Leeman BA, Frosch MP, Thiele EA.
Are cortical tubers epileptogenic? Evidence from electrocorticography.
Epilepsia.
2009;50(1):147-54.
PubMed abstract
Manohara D.
Primary care management of tuberous sclerosis complex in children.
J Am Acad Nurse Pract.
2012;24(7):391-9.
PubMed abstract / Full Text
Northrup H, Aronow ME, Bebin EM, Bissler J, Darling TN, de Vries PJ, Frost MD, Fuchs Z, Gosnell ES, Gupta N, Jansen AC, Jóźwiak
S, Kingswood JC, Knilans TK, McCormack FX, Pounders A, Roberds SL, Rodriguez-Buritica DF, Roth J, Sampson JR, Sparagana S,
Thiele EA, Weiner HL, Wheless JW, Towbin AJ, Krueger DA.
Updated International Tuberous Sclerosis Complex Diagnostic Criteria and Surveillance and Management Recommendations.
Pediatr Neurol.
2021;123:50-66.
PubMed abstract
Northrup H, Koenig MK, Pearson DA, Au KS.
Tuberous Sclerosis Complex.
GeneReviews® [Internet].
1993(Accessed Jun).
PubMed abstract / Full Text
Northrup H, Koenig MK, Pearson DA, Au KS.
Tuberous Sclerosis Complex.
GeneReviews.
2015.
PubMed abstract / Full Text
Northrup H, Krueger DA.
Tuberous sclerosis complex diagnostic criteria update: recommendations of the 2012 international tuberous sclerosis complex
consensus conference.
Pediatr Neurol.
2013;49(4):243-54.
PubMed abstract / Full Text
Key changes compared with 1998 criteria are the new inclusion of genetic testing results and reducing diagnostic classes from
three (possible, probable, and definite) to two (possible, definite). Additional minor changes to specific criterion were
made for additional clarification and simplification.
O'Callaghan FJ, Shiell AW, Osborne JP, Martyn CN.
Prevalence of tuberous sclerosis estimated by capture-recapture analysis.
Lancet.
1998;351(9114):1490.
PubMed abstract
Orlova KA, Crino PB.
The tuberous sclerosis complex.
Ann N Y Acad Sci.
2010;1184:87-105.
PubMed abstract / Full Text
Peron A, Au KS, Northrup H.
Genetics, genomics, and genotype-phenotype correlations of TSC: Insights for clinical practice.
Am J Med Genet C Semin Med Genet.
2018;178(3):281-290.
PubMed abstract
Peron A, La Briola F, Bruschi F, Terraneo S, Vannicola C, Previtali R, Perazzoli S, Morenghi E, Bulfamante G, Vignoli A, Canevini
MP.
Tuberous sclerosis complex (TSC), lymphangioleiomyomatosis, and COVID-19: The experience of a TSC clinic in Italy.
Am J Med Genet A.
2020;182(11):2479-2485.
PubMed abstract / Full Text
Prather P, de Vries PJ.
Behavioral and cognitive aspects of tuberous sclerosis complex.
J Child Neurol.
2004;19(9):666-74.
PubMed abstract
Seyam RM, Bissada NK, Kattan SA, Mokhtar AA, Aslam M, Fahmy WE, Mourad WA, Binmahfouz AA, Alzahrani HM, Hanash KA.
Changing trends in presentation, diagnosis and management of renal angiomyolipoma: comparison of sporadic and tuberous sclerosis
complex-associated forms.
Urology.
2008;72(5):1077-82.
PubMed abstract
Stuart C, Fladrowski C, Flinn J, Öberg B, Peron A, Rozenberg M, Smith CA.
Beyond the Guidelines: How We Can Improve Healthcare for People With Tuberous Sclerosis Complex Around the World.
Pediatr Neurol.
2021;123:77-84.
PubMed abstract
Thiele EA, Bebin EM, Bhathal H, Jansen FE, Kotulska K, Lawson JA, O'Callaghan FJ, Wong M, Sahebkar F, Checketts D, Knappertz
V.
Add-On Cannabidiol Treatment for Drug-Resistant Seizures in Tuberous Sclerosis Complex: A Placebo-Controlled Randomized Clinical
Trial.
JAMA Neurol.
2020.
PubMed abstract / Full Text
Tuberous Sclerosis Alliance.
Eye Involvement in Tuberous Sclerosis Complex.
Tuberous Sclerosis Alliance; (2006)
https://www.tsalliance.org/about-tsc/signs-and-symptoms-of-tsc/eyes/. Accessed on Sept. 2021.
Wataya-Kaneda M, Tanaka M, Hamasaki T, Katayama I.
Trends in the prevalence of tuberous sclerosis complex manifestations: an epidemiological study of 166 Japanese patients.
PLoS One.
2013;8(5):e63910.
PubMed abstract / Full Text
Wiznitzer M.
Autism and tuberous sclerosis.
J Child Neurol.
2004;19(9):675-9.
PubMed abstract

